Endometriosis has been consistently shown to decrease IVF success rates. Several mechanisms have been proposed to explain its negative impact, including reductions in egg quality and quantity, a hostile inflammatory environment in the fallopian tubes and surrounding tissue, immune dysfunction, and a less receptive uterine lining.
When outcomes fall short, the key clinical question facing patients and clinicians becomes: is the underlying issue mainly the “seed” (a non-viable embryo resulting from a low-quality egg) or the “soil” (a combination of factors preventing successful implantation of a viable embryo)? Distinguishing between the two is rarely straightforward — yet it is critical for guiding the next step in care.
MAGENTA™ provides objective insights into oocyte quality, helping clinicians clarify that distinction and make more targeted, confident decisions for what comes next.
- 35-year-old female G0P0 with Stage II endometriosis (history of chronic pelvic pain and laparoscopic confirmation of endometriosis)
- 3 years of primary infertility
- Ovarian reserve within expected range for age; normal male work-up
- Failed 3 cycles of IUI with ovarian stimulation
- IVF-ICSI planned
- 16 oocytes retrieved; 13 mature
- ICSI performed → 11 oocytes fertilized
- 6 blastocysts developed and were cryopreserved without PGT-A biopsy testing.
- All frozen embryos were graded as high quality using Gardner criteria and morphokinetic parameters assessed by time-lapse imaging.
- 4 FET cycles (two medicated, two modified natural cycle) were unsuccessful despite achieving adequate endometrial thickness.
- 2 embryos remain frozen.
- The patient has arranged a follow-up appointment to discuss next steps in her care.
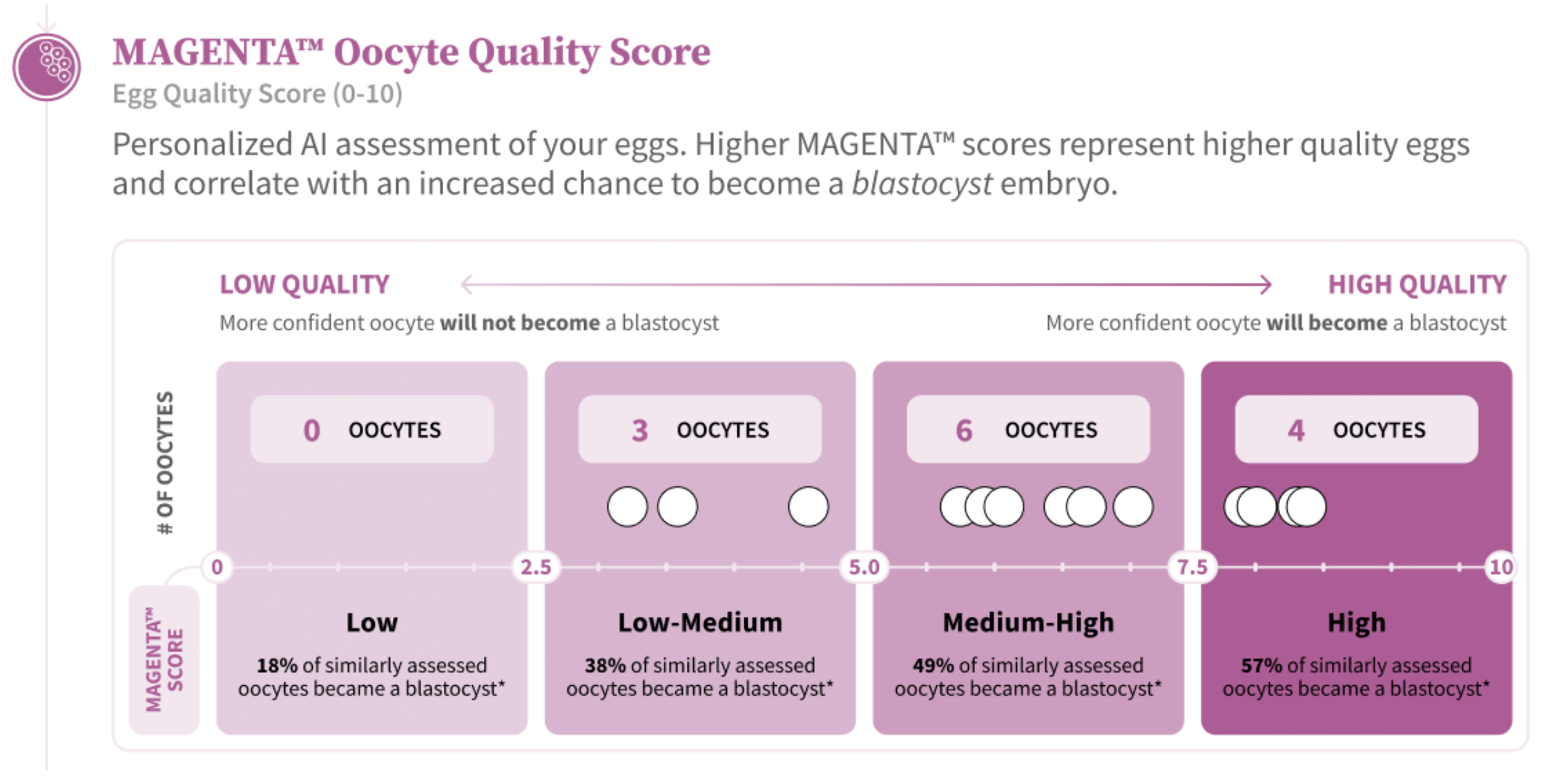
- The majority of oocytes are in the medium-high and high-quality ranges, with a smaller subset of low-medium scores.
- Interpretation: MAGENTA™ scores were consistent with age-related expectations and do not indicate a need for PGT-A testing of the remaining embryos.
In this endometriosis case, MAGENTA™ provided objective evidence supporting oocyte competence as unlikely to be the primary limiting factor — a finding consistent with the development of six high-quality embryos. Given the numerous unsuccessful FET cycles despite good embryo quality in a 35-year-old patient, the clinical focus now shifts more confidently toward endometrial receptivity as the likely contributor to failed implantation.
- Counselling: MAGENTA™ provided objective data supporting that egg quality was not the rate-limiting step, allowing the team to refocus the conversation on what was more likely contributing to her multiple failed FET cycles.
- Treatment planning: The focus shifted to the “soil” — prioritizing endometriosis-targeted FET preparation, including three months of hormonal suppression and additional progesterone support.
- Reducing trial-and-error: By helping to identify the most likely contributor to failed implantation, MAGENTA™ enabled more targeted decision-making — reducing the need for broad, empirical protocol changes and giving the patient a clearer path forward.
If you’ve found this example helpful in understanding how MAGENTA™ can be incorporated at your clinic or have feedback on other aspects related to your use of Future Fertility’s egg quality assessments, please share it with us at info@futurefertility.com.
You Might Also Like …
Join our mailing list for dispatches on the future of fertility

