When implantation fails in IVF, the key question becomes: is the issue the “seed” (embryo) or the “soil” (uterus)? MAGENTA™ provides objective insights into oocyte quality, helping to clarify that distinction. When oocyte scores are high, but implantation still fails, it can prompt a shift in focus toward uterine or other non-embryonic factors.
SAMPLE PATIENT CASE:
PATIENT BACKGROUND:
- 34-year-old female, G1P1, presented with recurrent implantation failure (RIF)
- She initially sought treatment for primary infertility and underwent a complete fertility workup, which was classified as unexplained.
- 12 oocytes retrieved
- 9 mature → 7 fertilized
- 3 high-quality blastocysts formed
- Outcome:
- 1 blastocyst transferred → healthy live birth
- 2 blastocysts cryopreserved
Two years later, she returned to grow her family. Both frozen embryos were thawed and transferred in two separate FET cycles, but neither resulted in implantation.
- 13 oocytes retrieved; 10 mature
- MAGENTA™ results: 4 oocytes of low-medium quality, 3 oocytes of medium-high quality, 3 oocytes of high quality
- ICSI performed → 8 oocytes fertilized
- 3 top-grade blastocysts developed (based on morphokinetics and grading)
- No PGT-A performed
- 1 fresh and 2 frozen embryo transfers were all unsuccessful
MAGENTA™ INSIGHTS: IDENTIFYING THE LIMITING FACTOR
THE MAGENTA™ REPORT:
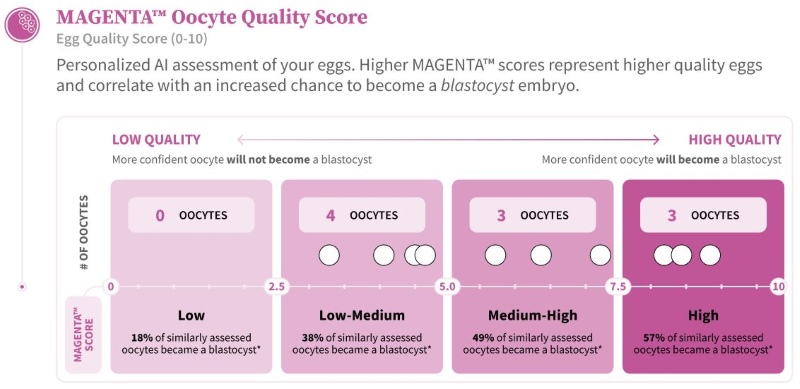
CLINICAL VALUE OF MAGENTA™ IN THIS CASE:
- Helps isolate the issue: In a 34-year-old patient with a prior live birth, high MAGENTA™ oocyte scores, and high-grade embryos based on morphological assessment, the findings—even in the absence of PGT-A—suggest a shift in clinical focus from the “seed” (embryo) to the “soil” (endometrium) as a potential limiting factor.
- Supports personalized care: Enables a more targeted evaluation of uterine factors, helping to avoid unnecessary repeat IVF cycles or premature consideration of donor gametes, such as donor eggs.
- Improves patient counselling: Provides a clear, data-driven rationale for recommending advanced endometrial testing, helping patients better understand the next steps in addressing recurrent implantation failure.
If you’ve found this examples helpful in understanding how MAGENTA™ can be incorporated at your clinic or have feedback on other aspects related to your use of Future Fertility’s egg quality assessments, please share it with us at info@futurefertility.com.
You Might Also Like …
Join our mailing list for dispatches on the future of fertility

